How do Hospitals Adapt during a Pandemic?
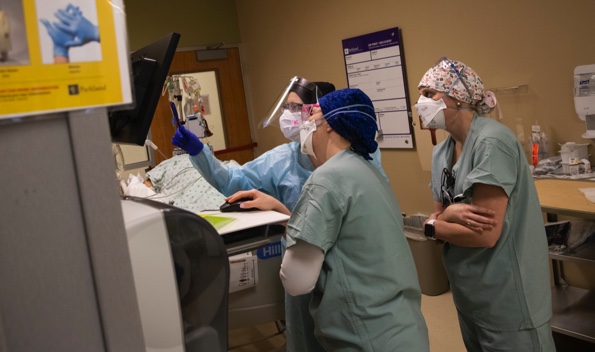
Throughout the COVID-19 pandemic, which has raged in the United States for just about two years now, we’ve seen how the lockdowns and sickness have affected the workplace, but how has it been affecting hospitals? How are the hospitals interacting with their community? And how have healthcare workers been keeping up with the constant flow of patients and information?
To learn about how hospitals have been adapting through the pandemic, I interviewed Dr. Geetanjali Srivastava who is a pediatric emergency medicine physician and the medical director of Valley Children’s Hospital in Fresno, California. Valley Children’s is one of the largest children’s hospitals in the country, serving about 1.3 million children and adolescents in the Central Valley of California, and over 100,000 children visit their emergency department each year. Dr. Geetanjali went to medical school at McGovern Medical School in Houston, did a three-year residency in pediatrics, and then a three-year fellowship in pediatric emergency medicine. She also has a Master’s Degree in Public Health with a focus on healthcare policy.
Author’s Note: This interview was edited for clarity.
Niraj: Because information on COVID was and still is rapidly evolving, how do healthcare workers and hospitals keep up with new information and filter through it? Is there a centralized way of getting information—is it standardized care—or do you have to decide for yourself and judge for yourself?
Dr. Geetanjali: That’s a really good question. The information was coming at us from everywhere, and some of the studies that were being published were really poor quality because people just wanted to get information out. We definitely felt overwhelmed by the information; it was really difficult to see patients and look at the literature as it was coming at you. I would say now and even then, the best place to go to is the CDC. We always use the WHO and CDC. I’m fortunate enough to work in a really good hospital with infectious disease specialists, so we really relied on them to keep up with the latest information and update us because their expertise is in novel viruses. I also work for an ER company, and we have just brilliant people in my company. Our chief medical officer took it upon himself and the education group in my company to send us information that they had sifted through, and they would send us a summary every week, which was so appreciated because we couldn’t be actively taking care of patients and reading all the literature. So, really, relying on people that aren’t actively seeing patients to get you the information was just paramount.
Niraj: But it sounds really rare to have someone giving you the information in a clear and concise way, right?
Dr. Geetanjali: Yeah, exactly. My chief medical officer is one of the smartest people I know, so I feel very fortunate. If it wasn’t for him and my group, it would have been the infectious disease specialists at the hospital. So I do think most hospitals probably did rely on the CDC and their internal support, but I felt that because ER doctors are frontline, to get information from an ER doctor was just essential for us to get through it. And initially there was not enough PPE, so we were getting information not just about how the virus spread but how to keep ourself safe and how to keep our family safe. They would tell us how we could recycle our N95s, which oven to put them in, what temperature to put them in, how to wash your clothes, how to come home, how to wipe down your car—they were telling us really practical things. At that time, we didn’t know if our families would be safe, so all of those things really kept us sane.
Niraj: So there’s a lot of pressure on infectious disease specialists to pump out the right information.
Dr. Geetanjali: Right, and even then a lot of it was unclear, so our ER doctors that were sifting through the information were giving us things that they had read about what was going on and worked in China, Italy, and New York. We were talking to people on the phone—talking to people in Italy. A lot of people were getting information from their own friends and families and acquaintances.
Niraj: I mean it’s a global network to try and figure out the information to best protect yourself and others.
Dr. Geetanjali: Yes, yeah.
Niraj: How does your hospital share data about the pandemic for national studies and statistics?
Dr. Geetanjali: A lot of things get reported to the state and our public health system. There are departments of health in every state, and there are diseases that are reportable. There’s a very clear list of what a hospital is mandated to report. Let’s use influenza as an example. We send our weekly data to a state lab and then that goes to a different part of the department of health so that we know what our epidemic of seasonal influenza is in California. Some information is mandated and some is voluntary, but we do this all the time for anything. Right now, we’re seeing a lot of respiratory syncytial virus (RSV), and every year we know the cases start around December. We follow trends, so we can predict when cases will peak, increase, or decrease. That kind of information is shared directly from hospitals and laboratories with our state health department.
Niraj: How does collaboration work for studies? Is information directly shared physician to physician? And how does it work if there are multiple hospitals participating in a study?
Dr. Geetanjali: To protect patient safety and confidentiality, all research has to be approved by an Institutional Research Board (IRB). Every hospital has an IRB, and if you’re doing a joint-study between many different hospitals, the protocol has to go through the IRB for each hospital to be approved. Because information needed to come out very quickly during the epidemic, these approval processes were expedited in my hospital, which I think was the case for most hospitals.
Niraj: How does your hospital reach out to the community to inform them about relevant public health issues? Does your hospital do it directly, or do you direct people to the CDC?
Dr. Geetanjali: We are very engaged with our community. Our hospital is very well-known and very well-respected. Some of the leaders of our hospital are leaders of the community, so we have done a lot of outreach. Our chief medical officer and chief executive officer have gone out in public and made public announcements, we have stuff on television, in print, we’ve had op-eds, we’ve advised school districts, we’ve had our infectious disease specialists on television and Facebook. The information is coming from the scientific community, especially the CDC, but we are able to give it by local experts and talk about our own experience in our hospital and our local community so making it specific and local is very important, especially as a children’s hospital in central California. Having the information come from people that live and work in your community is very important, but the actual information is the same as the CDC because that doesn’t change. We all have the same information—the same source of truth—but how we deliver it and engage with it is different.
Niraj: What is the proportion of healthcare workers at your hospital who are vaccinated against COVID-19? Does your hospital require vaccinations?
Dr. Geetanjali: When the vaccine was rolled out, and it was shown to be effective, it was initially volunteer, and it was the same all over the country. At our hospital when it was volunteer, we had 98% of the physicians accept the vaccine, and the 2% that didn’t might have had a medical exemption. Our hospital, and I think most hospitals, offered it to support staff—so anyone that wasn’t even in healthcare per se but supported the healthcare workers such as interpreters, cleaning people, administrators. The highest vaccination rate I think we got was 65% for the entire hospital. In the first few months of the vaccine rollout, there were very few side effects from the vaccine. As time went on, more and more hospitals stepped in to mandate vaccination for healthcare workers—the first was actually in Houston—because they knew that is the only way we can progress through the pandemic and keep everyone safe. And California was one of the first states to mandate vaccination for healthcare workers. So I would say at our hospital right now, the vaccination rate is probably in the high 90s, and the only people that are not vaccinated that continue to work are those who have a medical exemption—and they have to be tested on a weekly basis. So I would say it’s as close to 100% as you’re going to get.
Niraj: Why are vaccine mandates for healthcare workers necessary? Why can’t the vaccine be taken on a volunteer basis for healthcare workers?
Dr. Geetanjali: I think the mandate for healthcare workers is essential. If things get worse or there’s another pandemic, you need your workforce healthy. We cannot be replaced. Just to replace me would take another 20 years. You don’t want to lose your healthcare force. Every physician has at least 20 years of training, and same thing with nursing—we’re not robots. You have to keep yourself safe, and you have to keep the healthcare infrastructure safe. As we saw in New York when the first wave came through, there was a high mortality rate even for healthcare workers. It was frightening. We didn’t know what percent of the workforce would die because we didn’t know how deadly the virus was going to be. It was frightening, and that’s when you have to protect your healthcare workers. If the vaccine was more expensive and we didn’t have enough, you would still have to first vaccinate your first responders and then everyone else because if we don’t have first responders, we’re all in trouble.
Niraj: So how do healthcare professionals predict how COVID-19 will affect their community in advance? Do you use community positivity rate, hospitalizations, or ICU admissions as indicators?
Dr. Geetanjali: We use all three of those things, and luckily, the CDC and New York Times publish that. You look at trends and you learn from the experience of other regions that had been hit before you. We’re always learning from each other, so when New York was hit in the first wave of COVID-19, we knew about MIS-C because they started reporting it, and we got on phone calls with the doctors who reported seeing an “interesting inflammatory response.” Even when we started seeing it in California, it was literally word-of-mouth and people were publishing case reports. When we first saw it, it was exactly like what we had just read about two weeks ago.
Niraj: It’s so novel that you have to take in everything—
Dr. Geetanjali: Exactly. That’s where it’s so nice to have technology and have these colleagues around the country that are sharing information. So yeah, we follow all three indicators, and pediatric data is definitely different from adult data because we know that a smaller percentage of children will be affected by what adults are experiencing. But if there’s high adult mortality, we also expect the mortality rate to rise in pediatrics.
Niraj: So if you predict the cases will surge, what do you do to prepare your hospital?
Dr. Geetanjali: So initially, after what happened in New York, we developed different processes. One was doing medical screening exams in a tent away from the hospital to isolate people who had COVID-like symptoms to prevent infecting others in the hospital. If they were well-appearing, they would do a drive-by to see a physician or a nurse practitioner in all their PPE, and we do everything we need to do away from the hospital. If they were very ill, we could very quickly have them go to the main ER and be seen. We’ve also developed a process for COVID testing because we needed to test a lot of people. We came up with a process for testing that was outdoors, then we moved the process indoors. So we have been totally adapting to what we’re seeing, and we have enough shared processes across the country from our peers and our colleagues that we can share what’s worked somewhere else, try it, adapt it a little bit, and make it fit our own physical layout. I don’t know what the new variant will prove to be, but we’re going to be ready for it.
Niraj: I mean it’s like the epitome of science because you’re constantly taking in information, adapting it, changing it, and reporting it.
Dr. Geetanjali: Yeah, so true.
Niraj: What are some other instances where you had to make quick decisions and pivot quickly due to evolving circumstances?
Dr. Geetanjali: I feel like we pivoted so much on a daily basis because we were very proactive. When we heard what was going on in New York, even though California hadn’t experienced COVID at the time, we decided we were going to prepare to treat adults at our hospital in case adult hospitals were overwhelmed with COVID patients. One way we did this is we quickly stocked up on adult medicines that we don’t use in pediatrics, and we built that into our electronic medical record (EMR). We still have a tab in our EMR with adult drugs that is ready to be used if we ever need it. As ER doctors, we see adults on a normal basis even though it is not our expertise because adults in the hospital have accidents or strokes or heart attacks. We can treat, stabilize, and transfer adults. So when we realized kids aren’t getting sick in large numbers and there are so many adults that are going to need us, we wanted to figure out how we could potentially help take care of adult patients. We partnered with the rest of my company that had already been treating adults to learn what we could from them. And I had this information at my fingertips because my chief medical officer always shared it with me. We were very lucky, unlike New York, to be able to see what was coming and figure out how we would deal with it by seeing how COVID affected other areas before it hit us.
Niraj: What are major challenges children’s hospitals around the nation experienced or are experiencing right now from the pandemic?
Dr. Geetanjali: One thing I think everyone should know about is the nursing shortage. During the first wave of COVID-19, especially in New York, a lot of nurses, physicians, respiratory technicians, and medical technicians were exposed because we didn’t have enough PPE. There was a high mortality rate, and they took a lot of risk. They were also traumatized because they took care of a lot of people who couldn’t be visited by their loved ones during the last hours of their lives. They supported these families and being around people that are dying all the time takes a toll on you. If you talk to people that have gone through it, they’ll tell you how terrible it was to be the only person with these dying people that cannot be with their family. It took a huge toll on people, so a lot of nurses and other people in healthcare are just burnt out and are now looking for less stressful fields. This is a national trend, so a lot of hospitals now have no nurses and are relying on traveling nurses. Because of the demand, the salaries for traveling nurses have gone up to about triple or even quadruple what you normally pay for a nurse. Hospitals were already adversely affected financially from COVID-19 and now the workforce costs four times what it normally does, so hospitals are strained even more financially. But the hospitals are willing to pay that much just to get nurses to do the work. Currently in my ER, we are probably short about twenty nurses.
Niraj: And what is the total number of nurses you need?
Dr. Geetanjali: I don’t know because I don’t manage the nurses, but I would say we’re twenty nurses short at least. To replace them takes a long time, and even if we could get a traveling nurse, they don’t know the protocols, they don’t know our hospital, and they don’t know our systems. It is just so complicated that it takes a minimum of three to six months to onboard them properly. So you can imagine all that’s going on: everyone’s working really, really hard, nurses that are hired don’t know what they are doing because they haven’t had the chance to fully learn the processes, or we just don’t have enough nurses on shift. For example, if you have 70% of your nurses, 30% of the kids will never get into our beds. There have been days where we’ve had one in three patients that came to our emergency department leave without being seen because the wait was nine, ten, eleven, twelve hours long. Because we do not have enough nurses, a nurse could not bring new patients to a room to be seen by a physician, even though I had the bandwidth to see them as a physician, since we have ratios of one nurse to four patients.
Niraj: It’s a huge limiting factor for your work because you can’t do what you need to do.
Dr. Geetanjali: Absolutely. And that’s happening all over the country. If you can’t see 30% of the patients that came to see you, you feel like you’re not doing your job, so we’re all pretty stressed out about that. And the nurses that are working are working extremely hard because they know people are waiting that long. The families are also tired and exhausted‒who wants to wait twelve hours if they have a sick child? No one does. We’re in a really tough situation that most people don’t realize unless you go to the emergency department and see what’s going on. I don’t know when it’s gonna get better. It might be that some nurses have left the field forever and will never come back, and we don’t know how many people are going to go into nursing because it’s a tough job and not the highest paid job.
Niraj: What do you think we can do to make nurses feel more cared for because obviously they didn’t feel they were valued enough during the pandemic?
Dr. Geetanjali: I think as a country we need to respect teachers and nurses—people that we rely on. We don’t pay teachers and nurses what they should be paid, and we also don’t give them the respect they deserve. They’re not revered as they are in many Asian countries. In Japan, for instance, people bow to teachers because they know that they’re essential for society. Some of our teachers have been spit on and treated badly because they’ve asked a kid to wear a mask, and the same thing applies to nursing. I don’t know the answer. Obviously, their benefits and salaries should be raised, but I’m not sure if that’s going to bring them back. I don’t know all of the issues that affect nurses in particular, but they would definitely tell you. We just need to listen to them.
Niraj: What was your biggest failure as a hospital and as a leader during the pandemic?
Dr. Geetanjali: As a hospital, we could have been more visible early on in the pandemic. Most hospitals don’t want to play politics. Because of the way the Trump administration ran everything, hospitals were so afraid to play politics and take a stand that it wasn’t until much later in the pandemic that our hospital publicly made pro-vaccine and pro-PPE statements. Hospitals definitely were pro-vaccine and pro-PPE internally but not publicly. They didn’t want to be categorized as either blue or red, so they avoided the conversation. I think this was probably failed leadership. For me as a leader, I feel like I did everything: hours were cut because our volume went down significantly during COVID‒
Niraj: Why did the volume go down?
Dr. Geetanjali: First of all, people were really afraid to leave their home, and people weren’t getting sick all of a sudden. All the regular viruses and germs that people share in the winter stopped being shared because you were isolated with your nuclear family. People weren’t even getting hurt that much, so our volume dropped by 60%, just within about 2 weeks. I supported my team by giving them all my clinical hours, and I helped develop policies within my hospital, such as prioritizing who can get COVID-tested because our supply of tests was so limited. I did a multicenter study on MIS-C, and then I did a study with our entire hospital to see if people who were at most risk of exposure, my ER team, tested positive for COVID antibodies more than people that weren’t exposed to COVID patients such as hospital administrators because my fear was that my ER team had actually been infected and been asymptomatic, especially because in these early stages of the pandemic, the PPE was so limited.
I can say I tried to do scientific studies, I definitely did clinical, I did protocols, and I did policy. I don’t know what I would do about it, but I guess the only thing I failed on as a leader is that I have a lot of female doctors working for me, and I know they suffered a lot during the pandemic because they were working clinically, which was really mentally and physically tough, and they were going home and being teachers and doing zoom and helping their kids with their homework and still cooking and cleaning. They literally had zero minutes off a day, and I did not know what to do for them. I still don’t know how they got through that year, and I would love to know how to better support women. I just don’t know the right answer, and I don’t know if we as a community have one either. I still am in awe of my female physicians because they literally were on 24/7 for about a year and a half.
Niraj: It’s an interesting point you bring up because we usually think of healthcare providers like robots. We see them in their element providing medical care, but we don’t think of them dealing with the emotional impact and traumatic side of their job.
Dr. Geetanjali: Yeah. And luckily we weren’t seeing that many pediatric deaths because that would have just been a different dimension. But when we did see the MIS-C, we were hit emotionally. We didn’t know if MIS-C was going cause high mortality, so when we started the study, my team, which doesn’t really do a lot of research, was doing a lot to participate in this study and enroll patients because we all wanted to learn about MIS-C and understand why these kids are so sick because we had so many cases in Fresno. Nurses and physicians were so excited with this study because they all wanted to help.
Niraj: Just to go back to the emotional impact on healthcare workers, what resources do you and your colleagues have if you’re feeling burnt out, exhausted, traumatized, depressed, or anxious due to work?
Dr. Geetanjali: There are multiple layers of support. Luckily, we have a support system through my company which is the ER-group, and we also have it through our hospital. Our hospital has a lot of support services for physicians, and one way the hospital has supported us throughout the pandemic‒it sounds really silly, but it was so important‒is they fed us. They ordered food for physicians twice a week from local restaurants which supported both local restaurants that were shutting down and the physicians because we usually don’t eat. The hospital continues doing this even though the pandemic is waning because they know it keeps physicians happy and healthy, and us physicians get to see each other when we go and pick up the food which has been kind of nice. It sounds like such a small act, but it has been so meaningful. Another benefit the hospital offers is that they paid for every physician to be able to join this online meditation and exercise website for wellness. Internally in my company, we also have resources through our health insurance, we have lots of wellness events, and my company also sponsors webinars, so the support system is multimodal and pretty extensive.
Niraj: Are there psychologists at the hospital if you need them?
Dr. Geetanjali: Not on site, but you could access that very easily through your health insurance. There’s also a number that anyone in my company can call to get help, and the same thing with the hospital.
Niraj: To your knowledge, do other hospitals offer the same resources?
Dr. Geetanjali: I think they do. I’m talking solely for physicians, but I’m sure these resources are available for other staff members as well. As physicians, I don’t think we’re very good at asking for help, and I don’t think we’re really good at taking help, but I do know that at least in my hospital and my company, these topics are definitely discussed. You just have to take that one step of calling, but we can’t be reminded enough. Like maybe during every department meeting I should remind people about the phone number to reach support, so people don’t forget that they can always access help.
Niraj: What have you learned as a leader from the pandemic? In what ways do you think being a clinical leader has evolved during the pandemic?
Dr. Geetanjali: I think you can never have enough humility. It is essential to know what you don’t know and be really upfront about it, ask for help, and rely on other people for guidance. Also, it is important to know that you can make contributions in ideas using your prior experience in other aspects of life. You have more experience than you think you do. You have more ideas than you think you do. You have to share them and be open to other people’s ideas. You also must know that you can get through it. I will say my team and I were so brave. We didn’t know if we had enough PPE, and we didn’t know if we were going to be safe. I know there were other physicians that did not want to see COVID patients, and they were saying some pretty nutty things. But not one of my team members backed out. We were all like “Bring it on.” I think that’s ER-mentality. Everyone else doesn’t want to do this because it’s confusing, but we were like “We’ve got to do it. What’s the best way to do it?” We’re always solution-oriented. I was just really proud of the nursing leadership and my team leadership. We trusted each other, and we had each other’s backs. I really felt all the things I previously knew abstractly during the pandemic. My senior leadership above me were also there to support me, and I felt like they were listening to me more. It felt really good to keep my team safe and advocate for everyone in the ER. From the people that cleaned the rooms all the way to our physicians, I felt like I advocated for every single person that touched these patients and not just the physicians.
Niraj: And you also had to take into account people’s external situation outside of work, such as their kids and their mental health.
Dr. Geetanjali: Yeah absolutely. What my colleagues do at work is probably forty percent of their life, and my job as their boss is to make sure that at least what I can control at work is as good as it’s gonna get. I also need to know how I can support them in their private life and personal life to make sure they can go to soccer games and performances and things like that. I’m in charge of the schedule, so I make sure I have the soft part of being a boss there for them too. And it is my job to always think about my colleagues as a whole person, especially during COVID because it is so crazy stressful, especially for my female physicians.

Niraj is a current Senior at Keystone who is interested in spreading awareness about health issues and inequality through his writing. He is fascinated...
